Hello, everyone! This is without a doubt an update that we never thought we would be writing. If ever there was an “out of left field” update to my health journey, this may be it! It’s a long one that I’ve enjoyed writing. It’s been quite therapeutic to put this one out there. And in case you’re wondering, we now have clinical confirmation that I’m not right in the head!
What Happened?
In early February, I began experiencing some odd symptoms. I was picking up some of the kids from after school activities when I suddenly got very nauseous and experienced some mild paresthesia in the right side of my face (imagine you had some dental work done and the numbing medication is starting to wear off). We couldn’t help but wonder if we needed to do the stroke checklist, but a quick review of what was happening didn’t cause too much alarm. Symptoms subsided after a few hours. I made an appointment with my PCP for the following day.
The next day saw a return of the paresthesia accompanied by a mild headache, mild pain in my right leg, and a deep pain in my right elbow. All of these dissipated after an hour or so. I saw my PCP who did a cursory neurological exam. Luckily, the paresthesia and a little dizziness presented while I during my exam. My PCP was confident that I was having migraines and not a stroke. He gave me some migraine medication samples and told me to report back the next day to let him know if they worked. He mentioned that scans may be in my future if the drugs did not work. The symptoms persisted off and on over the course of a few days, but did respond to the migraine medication. The persistence was enough for my PCP to continue investigating the cause of the migraines. He ordered an outpatient MRI and advised that I keep taking the medication.
A Trip to the ED
We thought we had a plan. The MRI was scheduled. The drugs were working. We were going about life as usual and I had called Beth on my way home from work to ask if she wanted to go with me to the grocery store. I picked her up and we headed to the store. As we pulled into the parking lot, a bit of dizziness suddenly hit. I parked the car and told Beth what happened. I took the medication the doctor prescribed and we went about our shopping knowing it would take up to an hour for the drug to work.
Walking through the store was an adventure. The dizziness quickly became overwhelming. I was to the point that I could not walk without holding onto the cart, Beth, and/or the store shelves. Could we have been wrong? Was I possibly having TIAs (transient ischemic attacks) leading up to a stroke? We made the decision that this needed to be checked out and left the store with the Emergency Department as our next destination.
It’s an odd thing to be in a place where I have symptoms and side effects that I wouldn’t bat an eye over if I wasn’t on this cancer journey. Going to the ED to have things checked out has become a reality of my life as they could either be serious or nothing, but you have to check.
ED visits have become tolerable and somewhat predictable. I know that there is going to be waiting. I know that the bed is the least comfortable bed I’ve ever laid upon. I know that the drugs administered can make you feel more than a bit odd. To say that I couldn’t get anywhere near comfortable with telemetry wires and patches all over my abdomen, a blood pressure cuff, a pulse oximeter, and an IV would be an understatement. This visit was definitely the most discomfort I’ve felt since I had a bad drug reaction last summer. But I knew it would not last forever. They were quick to do an EKG and head CT. I was back in a curtained off bed before they could stick an IV in my arm. I wasn’t surprised when they ordered an MRI, but I was ready to go home. I was to the point where the discomfort made me question whether we should have come in the first place. That would quickly change.
We fully expected the ED doctor to say “Mr. Wright, you are not having a stroke. You’re having a migraine, but it’s good that you had this checked out…” Instead, the doctor said, “Mr. Wright, you are not having a stroke, we’re pretty sure you’re having a migraine, but the scans show a mass on your right occipital lobe that wasn’t on your previous scans. We’re going to admit you to the neuro floor.” By this point, my mom and dad were at the ED with us. Beth’s parents had our kids, and away we went up to the neuro floor at about 2:00 am.
The Neuro Floor
Here’s a fun fact that I wish I didn’t know. The Stryker beds at the hospital are much more comfortable than the Hill-Rom beds. I was beyond relieved when they wheeled me to a room with a Stryker bed waiting. I knew there was a chance I might get some rest.
I slept for a few hours with minimal interruptions for vitals and neuro checks. At about 6:00 am they came to get me for what I thought was going to be a repeat MRI. The doctors had changed the order to a head CT. It was quick and easy.
I tried to rest a bit after the CT, but I was awake at this point and couldn’t get back to sleep. We knew rounds were beginning and it was only a matter of time before a parade of doctors would come to see me. The day included a parade of visits from the hospitalist, a neurosurgery PA, a neurologist, my oncologist, occupational therapy, physical therapy, speech therapy, Beth’s parents, and our pastor (I texted him sometime in the morning). Beth was able to go home and rest for a bit. I was able to rest for a bit. There was another brain MRI. It became a full day.
DIAGNOSIS?
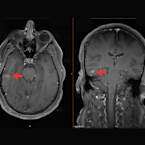
The big question we all have been wondering: what is going on. Unfortunately, we are not sure. We know that I have a mass in my right occipital lobe that measures approximately 5x6x8 mm. We know it has evidence of bleeding at some point. We’re confident the dizziness, paresthesia, etc. are indeed symptoms of new migraines. They shouldn’t be happening on the same side of the body as the mass, but they are (usually a problem on one side of the brain affects the other side of the body).
The doctors are now working to determine if this is a new tumor or a cavernoma (cavernous malformation of blood vessels). Neuroendocrine tumors rarely metastasize to the brain. A random cavernoma without preceding head trauma is also unusual. It’s going to take some time to determine what we’re dealing with and what to do about it.
In the meantime, my oncologist has fully transferred my care to a neuroendocrine tumor specialist. I have a follow-up brain MRI in a few weeks. We hope that the blood shown on the first scans will be reabsorbed by then and give us a better picture. There are surgical and radiation options available to treat the mass. I have a feeling we are going to have a few weeks of “hurry up and wait” followed by “hurry up and hurry up.”
Conclusion & Prayer Request
Brain metastasis of NETs are rare and usually a involve a poor prognosis. A cavernoma is treatable, but it’s never a great day when you have to operate on or radiate the brain. I’m also at an increased risk of stroke and seizure. We have a checklist of symptoms that would now require us to call EMS and have me taken immediately to the hospital by ambulance should they occur. I’m still dealing with the migraine symptoms on top of this. Vertigo has been insurmountable at times and I’ve already missed some work because of it. To once again quote Tom Petty, “the waiting is the hardest part.”
Please pray for my health. More so, please pray for Beth. She is living out our marriage vows to the full. More responsibility for the kids, chores, cooking, and life fall on her than normal. She also is caring for me on top of everything. Please pray for our kids. This whole experience has been unsettling for them. Please pray for our parents who have been filling the gaps for us when we cannot.
Finally, please pray for those who suffer who do not see the beauty of how our Lord works through suffering to help us love Him more. I remarked to a friend who texted me in the hospital that I was “out taking another stroll along the Way of the Cross.” I’ve said many times that this entire experience has been a great blessing in the sense that it has forced our family to reorient our priorities. I still have every hope for decades of life with Neuroendocrine Cancer, but the past few weeks are a sobering reminder that I might not. I want to become a saint. I don’t want to waste the time I have left on things that don’t matter. The Lord has worked through this Cross to draw me closer to Him and I am grateful for it. I look forward to sharing that message through some upcoming talks. Suffering is not wasted if it leads to a greater good. Don’t waste your suffering!
